Roadmap To Supports
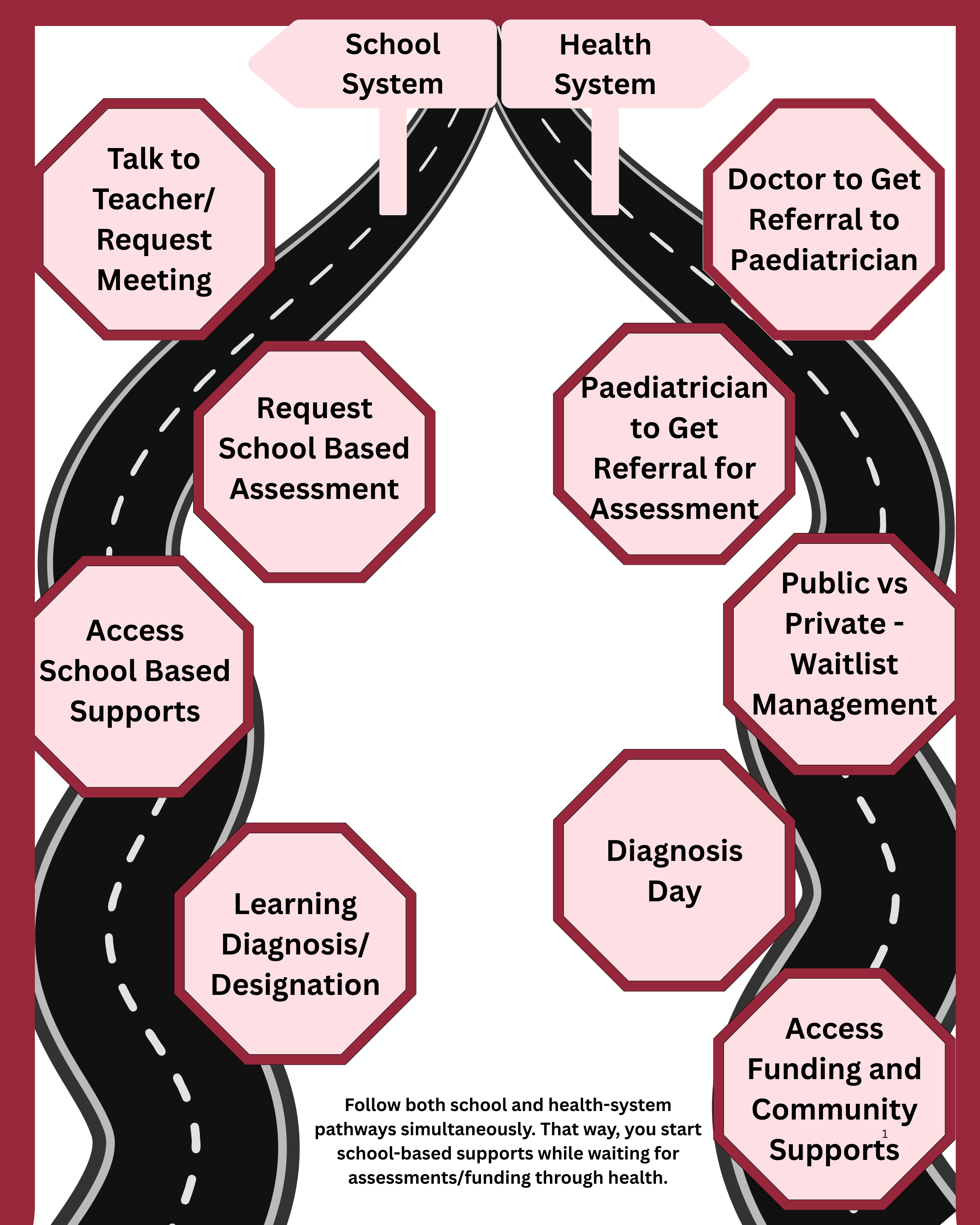
The Health System (Getting a Diagnosis)
You do NOT need a medical diagnosis to receive school supports.
-
Before you see a professional, you need data. Doctors see a snapshot; you see the whole picture.
The Logs: Keep a notebook of behaviour or communications that you think might support a diagnosis. Digital or paper is fine.
Record the where, when, the triggers, what happened afterwards and who was around to witness the behaviours or communications.
Example: "Tuesday 9am. Transition to school. Cried for 20 mins, refused to put on shoes. Calmed down with Mom giving a deep pressure hug and went to school."
School Data: Ask the teacher for any observations about behaviour and communications from your child at school. Request the teacher document anything they observe formally (email is best for a paper trail).
Video: Short clips (15-30 seconds) of the behaviours of concern can be more powerful than explaining them.
-
First thing to do is book an appointment to visit your Family Doctor, Nurse Practitioner (NP), or even a Walk-in Clinic to get a referral to a Paediatrician.
Seeing the Paediatrician:
Waitlists for seeing the Paediatrician vary.
Pro-tip: After a few weeks, once you know they have received the referral, call the office directly. Confirm they received the referral (this is an ongoing issue in our province) and request to be added to their cancellation list. This gets yourself on the booking clerks radar by politely communicating the appointment is urgent for your family.
The Paediatrician will likely have a report of your concerns from the referring doctor but you will be asked to go over it again in more detail. Present your concerns, backed by your evidence log.
Some Paediatricians may be comfortable with doing some diagnosis’ and treatments but they also may choose to refer you on for further or specialized assessment.
If the Paediatrician is unable to diagnose your child you can ask to be referred on to the appropriate specialized services or assessments.
Where they may refer you:
For Autism (ASD): They refer to BCAAN (BC Autism Assessment Network) / Sunny Hill Health Centre. Expect multidisciplinary assessments (the team may include psychologists, speech language pathologists, etc.)
For ADHD/Anxiety/Mood: They refer to a Child Psychologist, Child Psychiatrist or CYMH (Child & Youth Mental Health).
For Complex Development and Behaviours: They refer to the CDBC (Complex Developmental and Behavioural Conditions) program.
For Developmental Delay (Under 5): They refer to FVCDC (Fraser Valley Child Development Centre).
-
Public (Free via MSP):
Pros: Free. High quality multi-disciplinary teams.
Cons: Waitlists are long (often 12–24+ months for autism; 6–12 months for pediatricians).
Private (Pay out of pocket):
Pros: Fast (usually 1–4 months).
Cons: Expensive ($3,000–$5,000 for a Psych-Ed or Autism assessment).
Important: If you go private for Autism, you must ensure the clinician provides a "Non-BCAAN (Private) Diagnosis" that meets British Columbia Ministry of Health standards (typically requires a Psychologist and a Paediatrician/Speech Pathologist).
This expense may be partially funded by your extended health provider and can be used as a medical expense on your taxes.
-
Chronology of concerns and interventions (bullet points are always helpful!)
School reports, IEPs, previous therapy notes
Any prior test results or letters from specialists
A strengths list: what your child does well (helps assessments be balanced)
The School System (Getting Support and a Designation)
You do NOT need a medical diagnosis to start this process.
-
Step 1: Request a "School-Based Team" (SBT) Meeting
Do not just talk to the teacher at the door. Make it formal.
The Request Email: Email the teacher and principal requesting a School-Based Team (SBT) meeting and a school-based assessment (if it has not already started). Use factual language, name your concerns and attach your evidence log. Keep it short and sweet.
The Players: This meeting usually includes the Principal, Classroom Teacher, and the LST (Learning Support or Resource Teacher).
Pro-Tip: Bring a support person along for yourself!
The Meeting: In the meeting, do not just list symptoms. List educational impacts.
Weak: "He can't sit still."
Strong: "His inability to regulate his body means he is missing significant amounts of instructional time and has produced zero written output in three weeks."
The school is required to try interventions before testing. Remember to ask what interventions have been tried? Request that it is documented that they haven't worked so we can move to a higher level of testing immediately.
Paper trail = Accountability! Always follow up meetings with a polite summary email so you have documented requests and decisions.
-
Interim IEP: If the school agrees the child is struggling, they can create an IEP before a diagnosis exists. This is based on "needs," not "labels."
Language and Accommodations: Use specific and functional language. Avoid any vagueness. You can ask for whatever you believe might help your child. This could include things like visual schedules, body breaks, chunking work, or extra Teacher and EA staffing.
Pro-Tip: Be collaborative. Leave room for the school to suggest accommodations that they think would be beneficial from their perspective and for what will work within the classroom dynamics.
-
In BC, school assessments are broken down into three levels: Level A, B, and C. You typically have to "fail" or show need at one level to move to the next. There are also waitlists, often 1-2 years long, for some levels of assessments. You must prove the need to the School-Based Team (SBT).
Level A: Classroom Assessment (The "Teacher" Level)
Who does it: Classroom Teacher.
What it is: Observation checklists, reading benchmarks (PM Benchmarks), spelling inventories, and math snapshots.
Goal: To see if the child is within the class average.
Outcome: The teacher adjusts teaching style (e.g., moving the child to the front, giving extra time).
Level B: Academic Assessment (The "Learning Support" Level)
Who does it: Learning Support Teacher (LST) or Resource Teacher.
What it is: Standardized academic tests (e.g., KTEA, WIAT). These test achievement such as what grade level your child is reading, writing, or doing math at compared to thousands of other kids their age.
Goal: To prove the already suspected gap between the child's age and their ability.
Outcome: This is often enough to get an IEP started for academic struggles, even without a full diagnosis.
Level C: Psycho-Educational Assessment (The "Psychologist" Level)
Who does it: District School Psychologist.
What it is: The "Gold Standard" assessment. It combines the academic testing (Level B) with Cognitive Testing (IQ) to see how the brain processes information (working memory, processing speed, verbal reasoning).
Goal: To diagnose a Learning Disability (e.g., Dyslexia) or Intellectual Disability.
Outcome: A formal Ministry Designation (Category Q or K), which protects the child's right to support through graduation.
-
Schools use "Designations" (Ministry of Education Categories) to attach funding to a student.
Category Q (Learning Disability): Requires a Level C Psych-Ed assessment showing average intelligence but low academic performance.
Category K (Mild Intellectual Disability): Requires a Level C assessment showing low cognitive functioning (IQ approx. 50–70).
Category R (Moderate Behaviour Support): Does not require a diagnosis. It requires evidence that the student's behavior is disruptive and requires support.
Category G (Autism) / H (Intensive Behaviour): The school cannot give these designations without a medical diagnosis from a doctor or specialist first.
Review this Inclusive Education Funding Allocation - Category Checklist for further details.
Once you have the medical diagnosis, bring that report to the classroom teacher, LST or Resource Teacher.
The school psychologist reviews it and assigns a Ministry Designation (e.g., Category G for Autism, Category H for Intensive Behaviour).
Funding: designation triggers "Supplemental Funding" to the District (not the specific student). The District then pools this money to hire EAs and specialists to distribute support equitably.
Note: A diagnosis does not guarantee a full-time 1-on-1 EA.

